What is T1DM?
The Problem Type 1 diabetes (T1D)
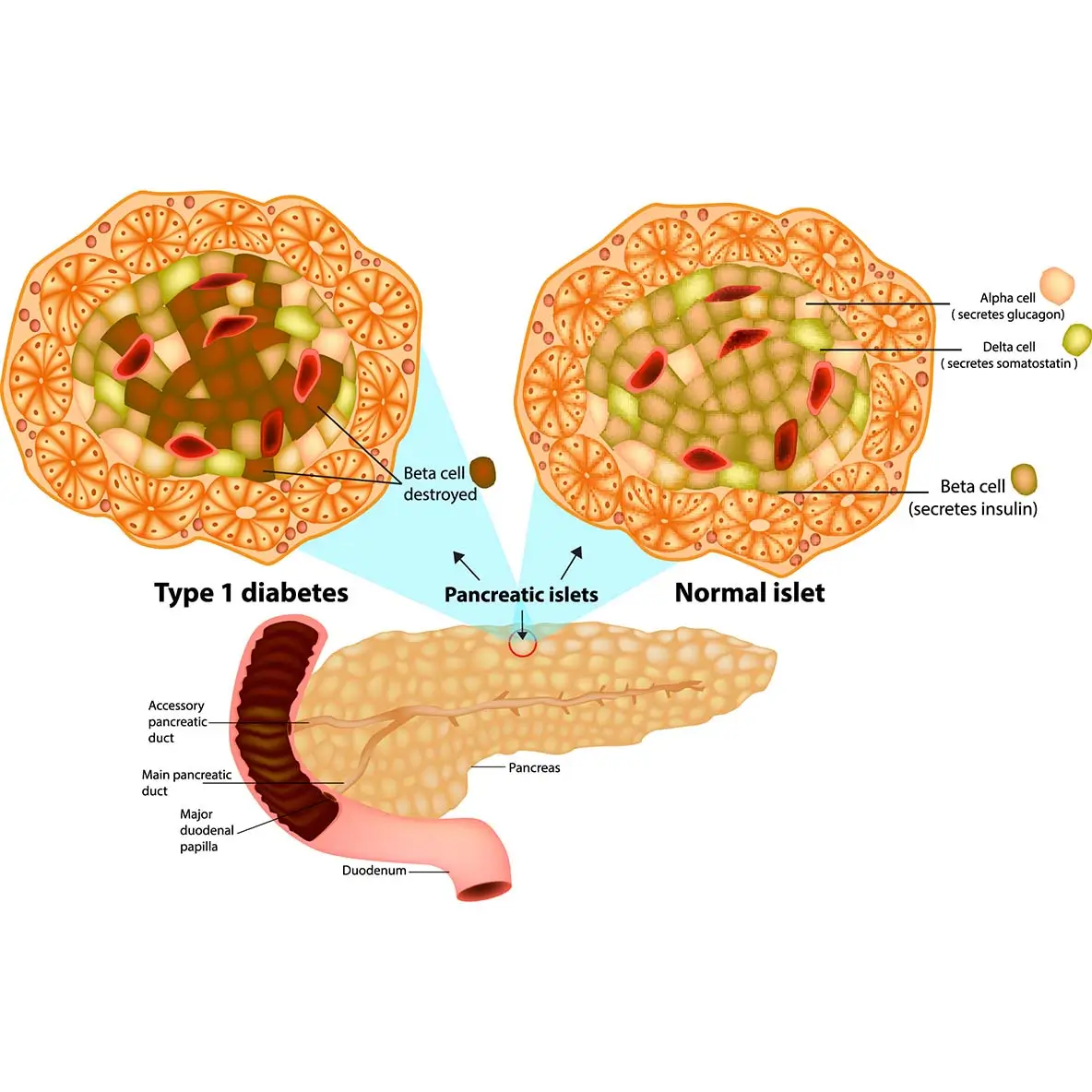
Type 1 diabetes (T1D) is the most common type of diabetes occurring in childhood and adolescence. Most cases of T1D are due to destruction of the pancreatic B-cells (which make insulin) by T-cells (white blood cells concerned with the immune system). This is a type of autoimmune destruction, wherein the body destroys part of itself. The B-cells are destroyed at a variable rate. Clinical symptoms of T1D occur when 90% or more of the cells are destroyed, so that sufficient insulin cannot be produced. In the absence of insulin, glucose in the blood is unable to move into the cells, and the blood glucose (BG) level rises while cells lack glucose to produce energy. This causes the person with diabetes to be tired, eat more, and yet lose weight.
Global Scenario of T1D
Type 1 Diabetes: The Indian Context
Especially in younger children, the incidence of T1D is observed to be increasing by 3% annually in India, where 70,000 new cases of the condition are reported each year. According to a report from Chennai City (an urban region) in 1996, the incidence was 10.5/100,000 people. In a separate survey from Karnal, Haryana, the prevalence was determined to be 26.6/100,000 in urban areas and 4.27/100,000 in rural regions, with an overall prevalence of 10.20/100,000 people.
Type 1 Diabetes: Causes
A hand-sized organ, the pancreas is situated behind the lower portion of the stomach. It creates digestive juices and hormones (endocrine function) (exocrine function). The endocrine cells are grouped together in the islets of Langerhans and consist of the ß-cells, which produce insulin, which regulates blood sugar and body fat levels, the a-cells, which produce glucagon, which raises blood sugar levels, and the d-cells, which sense blood sugar levels and relay that information to the a- and ß-cells. The immune system of the body targets and kills the ß-cells in T1D, which significantly reduces the amount of insulin produced. Insulin enables the body’s cells to take up glucose from the bloodstream and utilise it as an energy source. In the absence of insulin, the glucose remains in the blood stream, where it causes serious damage to all the organ systems of the body
People with T1D must take insulin in order to stay alive. Because insulin is a peptide which gets digested when it reaches the intestine, it must be injected into the body. Because insulin is needed to handle the glucose absorbed after food is eaten, it must be injected multiple times daily, or delivered multiple times through an insulin pump, before each major meal. In order to know how much insulin is needed, BG must be tested multiple times a day, by pricking a finger for a drop of blood. People with diabetes must also carefully balance their food intake and their exercise to regulate their BG levels, so that they avoid hypoglycemic (low BG) and hyperglycemic (high BG) reactions, which can be life threatening.
Type 1 Diabetes: Symptoms
Symptoms may develop suddenly over a few days, or gradually over days to weeks, and can vary from person to person.
T1D symptoms can surface quickly
and may include:-
- Unexplained weight loss
- Dry month
- Frequent urination
- Blurred vision
- Fatigue
- Sweet, or wine-like odor on breat
- Labored breathing; stupor
- unconsciousness
Classic symptoms include:
- Excessive thirst and water intake (POLYDIPSIA)
- Excessive urination (POLYURIA)
- Excessive food intake (POLYPHAGIA)
Type 1 diabetes is generally diagnosed in children, teenagers, or young adults, but can occur at any stage. Scientists know that autoimmune, genetic, and environmental factors are involved, but we do not yet know what exactly triggers the process off.

Prevention and Cure
To identify a long-term treatment for T1D, extensive research is being conducted all around the world. Since the discovery of insulin in 1922, numerous developments have been achieved that allow people with T1D to lead normal, fulfilling lives. But, there isn’t a cure accessible right now.
The types of insulin available for managing diabetes are:
The Rapid Acting Insulin
is used as bolus (given before each meal). Its’ action starts in 5-15 minutes, peaks in 30-60 minutes, and is over in 2-4 hours.
Short Acting Insulin
(also known as ‘regular’ or ‘plain’ insulin) starts acting in 30 minutes, peaks at 2-3 hours, and lasts for 5-6 hours.
Intermediate Acting Insulin
is a cloudy looking liquid, since insulin is in suspension: it starts in 2-4 hours, peaks at 4-8 hours, and lasts for 10 to 18 hours.
Long Acting Insulin
has a relatively peak-less action profile, lasting for about 12-24 hours. This is use to provide the basal needs of the body.
The amount and frequency of dosage is determined by the frequency of meals and the BG level. The child and family must learn how to monitor BG, how to load and inject insulin, and how to decide the dose of insulin. The doctor guides the family how to regulate the insulin doses based on the BG reading, the type and quantity of the meal to be taken, and the activity levels. Insulin can be taken by a syringe, a smaller convenient pen device, or by continuous subcutaneous insulin infusion (CSII) through a portable pump.
Precautions
- Insulin being a peptide, gets spoilt at temperatures below 2°C or above 25°C. Insulin should be kept in a cool environment, and never left in a vehicle or in the hold baggage of an aircraft.
- Predictable eating habits and activity levels make it easier to manage the BG well.
- Excessive sweets and oily food are harmful: not just the BG but also the blood pressure, and blood cholesterol levels increase with such foods.
- Fasting, e.g. during Ramzan and Navratri should be avoided by persons with T1D, as hypoglycemia can lead to coma, and even death.
- To avoid coma caused by hypoglycemia, persons with T1D should always carry an identity card and some sugar/ sweet candies in their pockets.
